Peripheral Nerves
Peripheral nerves form a highly specialized communication network of the PNS, linking the CNS to musculoskeletal tissues through bidirectional transmission of electrical signals. Structurally, they consist of axons organized into fascicles and supported by endoneurium, perineurium, and epineurium, ensuring mechanical protection and efficient action potential conduction.
Functionally, peripheral nerves integrate motor (efferent), sensory (afferent), and autonomic fibers. Motor output is executed via the neuromuscular junction (acetylcholine-mediated transmission), where neural signals regulate motor unit recruitment and rate coding, directly determining force production and timing of contraction. Sensory input from muscle spindles, Golgi tendon organs, and joint receptors provides continuous proprioceptive feedback, enabling real-time modulation of movement through spinal reflexes and higher central control.
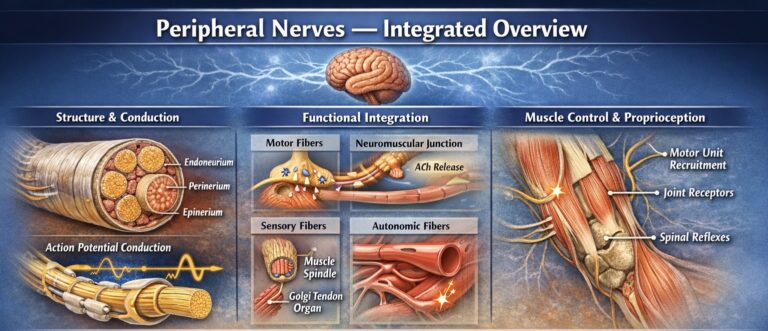
AI -generated illustration (MyoAnatomy)
Peripheral Nerve
Within a peripheral nerve, thousands of individual axons are arranged into fascicles and enclosed by multiple connective tissue sheaths. These structural layers collectively maintain the functional integrity of nerve fibers, facilitate vascular supply, and protect neural tissue during movement and mechanical loading within the musculoskeletal system.
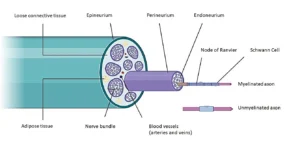
sdfbs
Nerve Fiber
The fundamental structural and functional component of a peripheral nerve is the axon, an elongated cytoplasmic extension of a neuron responsible for transmitting electrical impulses along the length of the nerve.
Axons vary in diameter, conduction velocity, and degree of myelination depending on their physiological function. Peripheral nerve fibers may therefore be classified into myelinated and unmyelinated fibers.
Unmyelinated Nerve Fibers
Unmyelinated fibers lack a continuous myelin sheath, although they may still be partially enveloped by Schwann cells. Because electrical impulses must propagate continuously along the axonal membrane, conduction velocity in these fibers is significantly slower.
Unmyelinated fibers are commonly involved in autonomic functions, pain transmission, and certain sensory modalities, where rapid conduction is less critical.
Myelinated Nerve Fibers
Myelinated fibers are surrounded by specialized glial cells known as Schwann cells, which produce the myelin sheath. Myelin is a lipid-rich insulating layer that wraps around the axon in multiple concentric layers.
The myelin sheath is interrupted at regular intervals by nodes of Ranvier, small gaps where the axonal membrane is exposed. Electrical impulses propagate rapidly between these nodes through a mechanism known as saltatory conduction, allowing nerve signals to travel at high speeds.
Overview
Peripheral nerves are supported by several concentric layers of connective tissue that provide structural protection, mechanical resilience, and metabolic support. These layers include the endoneurium, perineurium, and epineurium, which collectively form the connective tissue framework of the nerve.
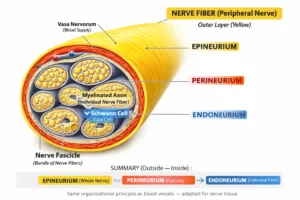
AI -generated illustration (MyoAnatomy)
Endoneurium
Innermost connective tissue layer of a peripheral nerve, enclosing individual nerve fibers (axons with their Schwann cells) and separating them from one another within a fascicle. It forms the smallest structural unit of nerve organization, lying deep to the perineurium and epineurium.
Anatomically, it consists of delicate loose connective tissue that runs longitudinally along the nerve, allowing slight mobility and alignment of fibers while accommodating mechanical stress during movement. It contains a fine capillary network derived from the vasa nervorum, ensuring local metabolic support of each fiber.
Functionally, the endoneurium provides structural support, maintains an organized conduction pathway, and protects individual axons from compression and deformation, thereby preserving efficient nerve impulse transmission.
Perineurium
Specialized connective tissue sheath that surrounds groups of nerve fibers, organizing them into fascicles and forming the intermediate layer between endoneurium and epineurium.
It consists of concentric layers of perineurial cells that establish a tight junction–based barrier, constituting the principal component of the blood–nerve barrier.
Functionally, it provides mechanical strength and fascicular compartmentalization, protecting against stretch and compression while maintaining a controlled internal environment essential for stable axonal conduction.
Epineurium
Outermost connective tissue sheath that encloses multiple fascicles and their vascular supply into a single nerve trunk.
Composed of dense irregular connective tissue, it provides global mechanical protection and compliance, allowing the nerve to tolerate stretch and displacement.
It houses the vasa nervorum, ensuring vascular continuity, and permits controlled fascicular mobility, thereby distributing mechanical forces and preserving overall nerve integrity.
Functional Significance
The hierarchical arrangement of axons, fascicles, and connective tissue layers ensures that peripheral nerves can efficiently transmit electrical signals while remaining protected from mechanical and metabolic stress.
This structural organization allows nerves to maintain their functional integrity as they travel through the body, often passing through muscular compartments, fascial planes, and joint regions where movement and mechanical forces are constantly present.
Through this integrated structure, peripheral nerves maintain the precise neural communication required for motor control, sensory perception, and autonomic regulation within the musculoskeletal system.
Overview
Peripheral nerves are functionally heterogeneous mixed structures composed of motor (efferent), sensory (afferent), and autonomic fibers that connect the central nervous system with peripheral tissues. Within a single nerve trunk, these fiber types are organized into fascicles and conduct impulses bidirectionally, enabling continuous integration of movement, sensation, and autonomic regulation.
Through this coordinated activity, peripheral nerves support skeletal muscle contraction, proprioceptive feedback, vascular control, and reflex function, forming an integrated system for precise neuromuscular and physiological regulation.
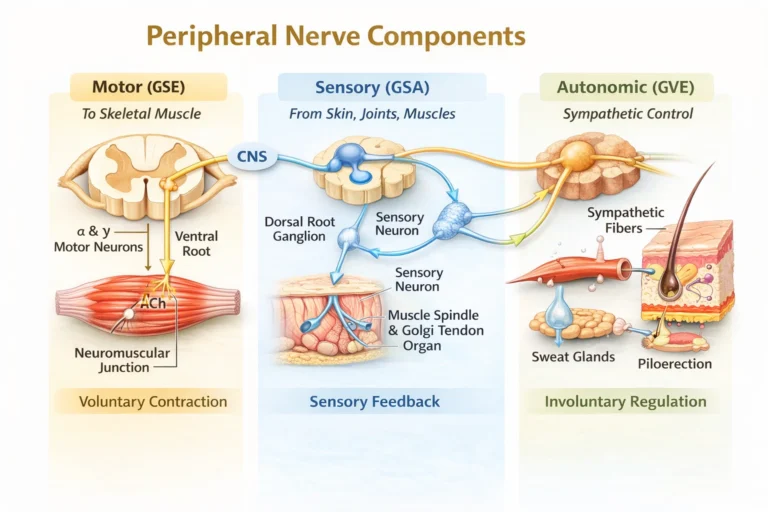
AI -generated illustration (MyoAnatomy)
Motor Fiber
Motor (GSE, somatic efferent) fibers transmit impulses from the central nervous system to skeletal muscle, forming the final common pathway of motor output. They arise from alpha and gamma lower motor neurons in the anterior (ventral) horn of the spinal cord (or brainstem motor nuclei), exit via ventral roots, and travel within peripheral nerves to their target muscles.
Axons terminate at neuromuscular junctions, where acetylcholine release induces depolarization and initiates excitation–contraction coupling.
Functionally, motor fibers mediate voluntary contraction, muscle tone, and coordinated movement (alpha motor neurons), while gamma motor neurons regulate muscle spindle sensitivity, enabling proprioceptive control and reflex modulation.
Sensory Fiber
Sensory (GSA, afferent) fibers transmit information from peripheral receptors to the central nervous system, providing continuous feedback on the mechanical and physiological state of tissues. They arise from pseudounipolar neurons in the dorsal root ganglia, with peripheral processes extending to receptors in skin, muscles, tendons, and joints, and central processes entering the spinal cord via dorsal roots.
These fibers convey multiple modalities, including mechanoreception (touch, pressure, vibration), proprioception (muscle length, tension, joint position), nociception (pain), and thermoreception (temperature).
Functionally, sensory fibers provide
Autonomic Fiber
Autonomic (GVE, visceral efferent) fibers within peripheral nerves regulate involuntary functions of vascular and cutaneous structures, predominantly via the sympathetic system in the limbs. These fibers originate from preganglionic neurons in the spinal cord, synapse in autonomic ganglia, and reach target tissues as postganglionic fibers traveling with peripheral nerves.
They control key functions including vasomotor tone (vascular diameter), sudomotor activity (sweat secretion), and piloerection (arrector pili muscles), as well as local regulation of tissue perfusion.
Functionally, autonomic fibers maintain vascular homeostasis and thermoregulation, adjusting blood flow and skin responses to meet metabolic demands, particularly during exercise and environmental stress, thereby supporting optimal tissue function.
Functional Significance
Peripheral nerves are mixed structures containing motor (GSE), sensory (GSA), and autonomic (GVE) fibers, enabling bidirectional communication between the CNS and peripheral tissues.
A single nerve provides motor output, sensory feedback, and autonomic regulation of vascular tone and metabolism. This forms a closed-loop system in which afferent input – via spinal and supraspinal integration – modulates efferent activity, ensuring precise control of movement, tone, and posture.
Functionally, peripheral nerves act as integrated neurovascular units coordinating movement, sensation, and tissue homeostasis
Motor Control
Peripheral nerves provide the motor interface between the central nervous system and skeletal muscle, enabling controlled force generation through alpha motor neuron discharge and neuromuscular junction (acetylcholine-mediated) transmission. This initiates excitation–contraction coupling within muscle fibers, leading to mechanical force production.
Regulation of motor unit recruitment and rate coding determines force magnitude, timing, and gradation, allowing precise execution of movement, joint stabilization, and maintenance of posture.
Sensory Feedback
Peripheral nerves transmit continuous afferent input from musculoskeletal receptors to the CNS, forming the basis of proprioceptive control. Muscle spindles encode changes in length and velocity, Golgi tendon organs monitor tension, and joint mechanoreceptors detect position and load.
This input is processed at both spinal and supraspinal levels (including cerebellar integration), enabling real-time modulation of motor output and maintaining accuracy, coordination, and adaptability of movement.
Reflex regulation
Peripheral nerves mediate spinal reflex circuits that provide rapid, automatic responses independent of conscious control. Reflexes such as the stretch reflex regulate baseline muscle tone and postural stability, while withdrawal reflexes protect against harmful stimuli.
These mechanisms operate through tightly regulated sensorimotor loops, ensuring immediate neuromechanical adjustment and protection against excessive mechanical stress or injury.
Neuromechanical Integration
Peripheral nerves function as a closed-loop neuromechanical system, integrating motor output, sensory feedback, and reflex activity into coordinated movement. This system maintains neuromechanical coupling, allowing efficient force transmission, balance, and adaptation to changing mechanical demands.
Disruption of peripheral nerve function results in denervation, impaired excitation–contraction coupling, altered feedback gain, and loss of coordinated motor control, leading to weakness, atrophy, instability, and inefficient movement patterns.
Peripheral Nerve Injury
Peripheral nerve dysfunction arises from disruption of axonal conduction and neural integrity, impairing bidirectional signal transmission between the CNS and musculoskeletal tissues.
Common mechanisms include mechanical compression (entrapment), traumatic injury (stretch, laceration), inflammatory processes, and metabolic disorders. These insults may cause demyelination (slowed conduction) or axonal degeneration (loss of signal transmission), leading to impaired excitation–contraction coupling and defective sensory signaling.
Additionally, compromised microvascular supply via the vasa nervorum contributes to ischemic nerve injury, further exacerbating dysfunction.
Motor Disfunction
Damage to motor fibers disrupts alpha motor neuron output, resulting in reduced or absent muscle activation. This leads to weakness, paralysis, and impaired motor unit recruitment, ultimately compromising force generation and joint stability.
Prolonged denervation results in muscle atrophy and loss of neuromuscular efficiency, transforming movement into a mechanically unstable and energetically inefficient process.
Clinically, this is evident in conditions such as radial nerve injury (wrist drop), where loss of extensor function severely alters upper limb biomechanics.
Sensory Loss
Sensory fiber involvement disrupts transmission of afferent signals from mechanoreceptors and nociceptors, leading to loss of proprioception, impaired coordination, and altered movement accuracy.
Without adequate feedback, the CNS cannot effectively modulate motor output, resulting in ataxia and instability. Simultaneously, nerve irritation or damage may generate neuropathic pain, characterized by abnormal signaling within sensory pathways.
Conditions such as carpal tunnel syndrome (median nerve compression) and sciatica (sciatic nerve irritation) illustrate how sensory dysfunction produces both pain and impaired motor control.
Neuromechanical Dysfunction
Peripheral nerve dysfunction represents a failure of the neuromechanical control system, disrupting the integration of motor output, sensory feedback, and reflex regulation.
This leads to combined deficits in strength, coordination, and adaptive control, significantly impairing functional movement. Systemic conditions such as peripheral neuropathy further exacerbate this by causing diffuse nerve damage and progressive functional decline.
Clinically, accurate diagnosis requires understanding nerve anatomy and physiology to localize lesions, differentiate motor vs sensory deficits, and guide targeted rehabilitation or intervention strategies.
