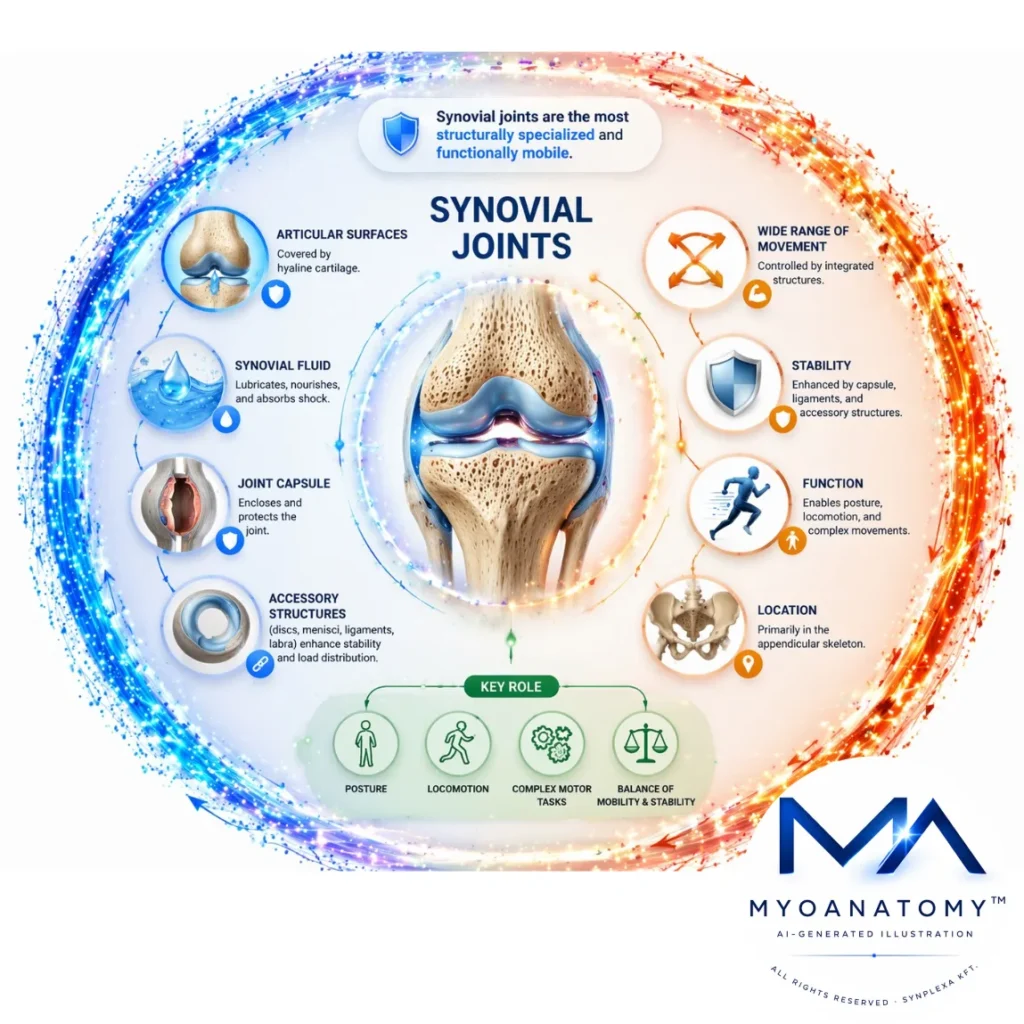
Synovial Joints
Synovial joints are the most structurally specialized and functionally mobile class of joints, characterized by a synovial cavity separating articular surfaces covered by hyaline cartilage. Synovial fluid within the cavity enables lubrication, nutrient diffusion, and shock absorption, ensuring low-friction movement.
In contrast to fibrous and cartilaginous joints, they allow a wide range of controlled movements through an integrated system of capsule, synovial membrane, ligaments, and accessory structures (e.g., discs, menisci, labra) that enhance stability and load distribution.
Functionally, synovial joints are essential to the locomotor system, enabling posture, locomotion, and complex motor tasks by balancing mobility with stability. Their biomechanics rely on coordinated interactions between cartilage, synovial fluid, periarticular tissues, and neuromuscular control.
They are primarily located in the appendicular skeleton, where large ranges of motion are required, and are structurally adapted to efficiently transmit forces while minimizing wear during repetitive loading.
STRUCTURAL COMPONENTS
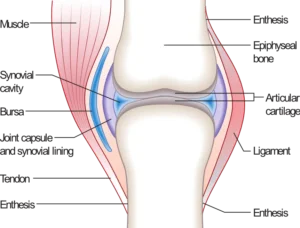
Synovial Joint Example (Joint.png)” – Madhero88, via Wikimedia Commons. Licensed under CC BY SA 3.0
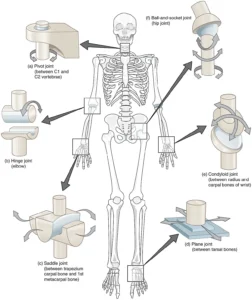
“Types of Synovial Joints” by OpenStax College, from Anatomy & Physiology, via Wikimedia Commons.
Licensed under CC BY 3.0
Articular Cartilage
Articular cartilage in synovial joints is a specialized form of hyaline cartilage composed predominantly of type II collagen fibrils embedded within a highly hydrated proteoglycan-rich extracellular matrix. Chondrocytes are sparsely distributed within lacunae and maintain matrix homeostasis through tightly regulated synthesis and degradation.
This tissue is avascular, aneural, and alymphatic, relying entirely on diffusion from synovial fluid for nutrient supply and waste removal. It exhibits a zonal organization (superficial, transitional, deep, and calcified layers), each adapted to specific mechanical functions, including shear resistance at the surface and compressive load absorption in deeper regions.
The extracellular matrix provides viscoelastic properties, allowing deformation under load and recovery upon unloading, thereby distributing forces efficiently and protecting the underlying subchondral bone while maintaining a low-friction articulating surface.
Exam Question
Explain how the zonal architecture and extracellular matrix composition of articular cartilage enable it to withstand both compressive and shear forces while remaining avascular.
Synovial Cavity
The synovial cavity is a fluid-filled space separating the articular surfaces, essential for frictionless joint movement. It contains synovial fluid, a plasma-derived ultrafiltrate enriched with hyaluronic acid and lubricin, which provides lubrication, reduces wear, and facilitates nutrient diffusion to avascular articular cartilage.
Synovial fluid exhibits non-Newtonian, shear-thinning behavior, allowing it to adapt to varying mechanical demands – becoming less viscous during rapid movement to reduce friction, and more viscous at rest to enhance joint stability.
The cavity is enclosed by a fibrous capsule lined internally by the synovial membrane, which regulates fluid composition and maintains joint homeostasis. Through continuous circulation and pressure changes during movement, synovial fluid supports metabolic exchange and contributes to shock absorption and load distribution.
Exam Question
Analyze how the biochemical composition and rheological properties of synovial fluid contribute to both lubrication and nutrition of articular cartilage in synovial joints
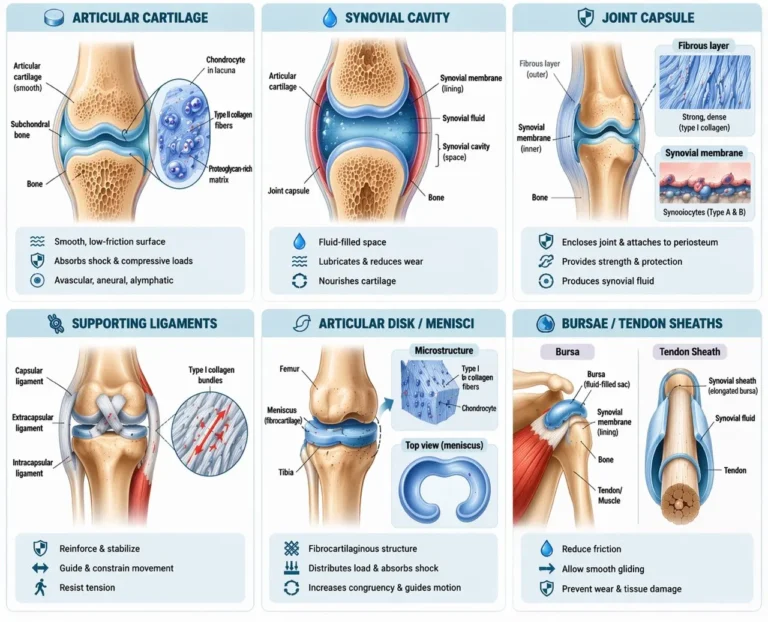
AI-Generated Illustration MyoAantomy
Joint Capsule
Each synovial joint is enclosed by a joint capsule forming a continuous sleeve between adjacent bones and blending with the periosteum. It consists of two structurally and functionally distinct layers.
The outer fibrous layer is composed of dense irregular connective tissue rich in type I collagen, arranged to resist multidirectional mechanical stresses. It provides tensile strength, structural containment, and limits excessive joint movement.
The inner synovial membrane is a specialized connective tissue lacking a true epithelium and containing synoviocytes. Type A synoviocytes perform phagocytic functions, while Type B synoviocytes synthesize synovial fluid components, including hyaluronic acid and lubricin, maintaining the biochemical environment of the joint.
This dual-layered organization ensures both mechanical stability and metabolic regulation of the intra-articular space, enabling efficient movement while preserving joint integrity.
Exam Question
Explain how the structural differences between the fibrous capsule and synovial membrane contribute to both mechanical stability and metabolic homeostasis in synovial joints.
Supporting Ligaments
Ligaments are dense connective tissue structures that reinforce synovial joints and integrate with surrounding musculoskeletal components to guide and constrain movement.
They are classified based on their anatomical relationship to the joint capsule: capsular ligaments (thickenings of the fibrous capsule), extracapsular ligaments (external to the capsule), and intracapsular ligaments (located within the capsule but excluded from the synovial cavity).
Ligaments are primarily composed of type I collagen fibers arranged in parallel bundles aligned with dominant mechanical stress vectors. This organization allows controlled elongation under tension while resisting excessive displacement, contributing to joint stability and directional control of movement.
Functionally, ligaments act as passive stabilizers, limiting abnormal motion, maintaining joint congruency, and providing proprioceptive feedback through embedded mechanoreceptors.
Exam Question
Analyze how the collagen fiber orientation and anatomical positioning of ligaments determine their role in guiding joint motion and preventing instability.
Articular Disk/Menisci
Certain synovial joints contain fibrocartilaginous intra-articular structures – articular discs and menisci – composed predominantly of type I collagen arranged to resist multidirectional mechanical stresses. These structures may partially or completely divide the synovial cavity, creating functionally distinct compartments within a single joint.
Their morphology is joint-specific: crescent-shaped menisci in the knee enhance congruency between incongruent surfaces, while complete discs (e.g., temporomandibular joint) allow complex combined movements. The organized collagen architecture enables resistance to compressive, tensile, and shear forces.
Functionally, discs and menisci optimize load distribution, increase joint stability, guide movement, and reduce focal stress by improving articular congruency and dissipating mechanical energy across the joint surface.
Exam Question
Explain how the fibrocartilaginous composition and structural organization of articular discs and menisci contribute to load distribution and joint stability in synovial joints.
Bursae/Tendon Sheets
Bursae are discrete synovial fluid-filled sacs located at sites of friction between soft tissues and bone or adjacent structures. They are lined by a synovial membrane-like layer and contain a thin film of lubricating fluid that reduces mechanical resistance during movement.
Tendon sheaths are specialized elongated bursae that envelop tendons, particularly where they traverse confined spaces or pass over osseous prominences. They facilitate smooth gliding of tendons while maintaining alignment and reducing wear.
Together, these structures form an integrated system of friction-reducing interfaces within the musculoskeletal system, minimizing energy loss, preventing tissue damage, and enabling efficient, repetitive movement.
Exam Question
Analyze how bursae and tendon sheaths contribute to reducing friction and preserving mechanical efficiency in regions of high repetitive motion.
FUNCTIONAL ROLE
Controlled Mobility
Synovial joints constitute the principal articulations enabling a wide spectrum of skeletal kinematics required for posture, locomotion, and manipulation. Their architecture permits movement across defined degrees of freedom, determined by articular surface geometry and constrained by passive (capsule, ligaments) and active (musculotendinous) stabilizers.
Unlike fibrous and cartilaginous joints, synovial joints allow substantial motion while preserving mechanical coherence. This controlled mobility reflects a regulated balance between articular congruency, capsuloligamentous constraint, and neuromuscular control, ensuring efficient movement without loss of joint integrity.
Force Transmission
Synovial joints function as critical biomechanical interfaces that convert muscle-generated force into joint torque and coordinated skeletal motion. Muscular contraction is transmitted via tendons across the joint, where it is transformed into angular rotation or translational displacement.
This mechanism integrates individual skeletal segments into coordinated kinetic chains, allowing forces to be distributed and modulated across the limb or trunk. As a result, movement is mechanically linked rather than isolated, optimizing efficiency and minimizing localized overload.
Friction reduction
A defining characteristic of synovial joints is their capacity to sustain near-frictionless articulation under physiological loading conditions. Articular cartilage provides a highly specialized low-friction surface, while synovial fluid facilitates both boundary and fluid-film lubrication, as well as metabolic exchange.
These mechanisms enable joint surfaces to tolerate repetitive compressive, shear, and translational stresses while redistributing mechanical loads over a wider contact area. This reduces stress concentration, protects subchondral bone, and preserves long-term joint function.
Dynamic Stability
The functional performance of synovial joints depends on a dynamic equilibrium between mobility and constraint. Excessive rigidity limits kinematic efficiency, whereas excessive laxity compromises alignment and effective force transmission.
Dynamic stability arises from the coordinated interaction of articular geometry, capsuloligamentous structures, muscle tone, and tendon forces. This integrated system enables joints to maintain alignment under load while permitting controlled motion, ensuring resistance to displacement without sacrificing functional mobility.
CLINICAL RELEVANCE
Degenerative Joit Failure
Synovial joints are chronically exposed to repetitive mechanical loading, rendering them susceptible to degenerative failure. In osteoarthritis, progressive breakdown of articular cartilage disrupts the low-friction, load-bearing interface, leading to altered stress distribution and increased mechanical strain on subchondral bone.
This results in pain, stiffness, and reduced mobility. Importantly, degeneration represents not merely cartilage loss, but failure of the joint as an integrated biomechanical system, with secondary changes including subchondral sclerosis, osteophyte formation, and impaired force transmission.
Sinovial Inflamation
The synovial membrane is central to joint homeostasis but also a primary site of pathology in inflammatory joint disease. In rheumatoid arthritis, persistent immune-mediated inflammation induces synovial hyperplasia and formation of pannus—a proliferative, invasive tissue that erodes cartilage and adjacent bone.
This process disrupts the synovial environment, leading to progressive joint destruction, deformity, and instability. It exemplifies how alteration of synovial regulation can compromise the entire articulation, transforming a controlled mechanical system into a site of structural failure.
Joint Instability
Normal synovial joint function depends on the integrity of passive stabilizers, particularly the joint capsule and ligaments, as well as active neuromuscular control. Injury to these structures, such as ligamentous rupture or capsular laxity, alters joint kinematics and reduces resistance to abnormal displacement.
This leads to instability, characterized by impaired alignment and inefficient force transmission across the joint. Chronic instability predisposes to recurrent injury, altered loading patterns, and progressive degenerative changes.
Joint Dislocation
Synovial joints, by virtue of their mobility, are vulnerable to acute structural disruption. Dislocation occurs when stabilizing forces are overcome, resulting in complete loss of congruency between articulating surfaces.
This causes immediate loss of function and often involves damage to surrounding structures, including ligaments, capsule, and neurovascular elements. Dislocation disrupts normal force transmission and joint mechanics, and if not properly reduced and stabilized, may lead to long-term instability and degenerative joint disease.
